When Stress Meets the Gut: How PTSD Shapes IBS Symptoms Through the Brain–Gut Axis
Understanding Impacts of Stress and Trauma on IBS
While acute (short-lived) stress is unlikely to cause lasting harm, chronic stress (persisting over long periods) places continuous strain on physiological systems, increasing disease risk, immune dysregulation, and health-damaging behaviors. Trauma is defined as the exposure to stressful events that involve death, serious injury, or sexual violence, which can lead to Post-Traumatic Stress Disorder (PTSD), a mental health condition resulting from exposure to traumatic events that creates intense feelings of fear, helplessness, or horror.
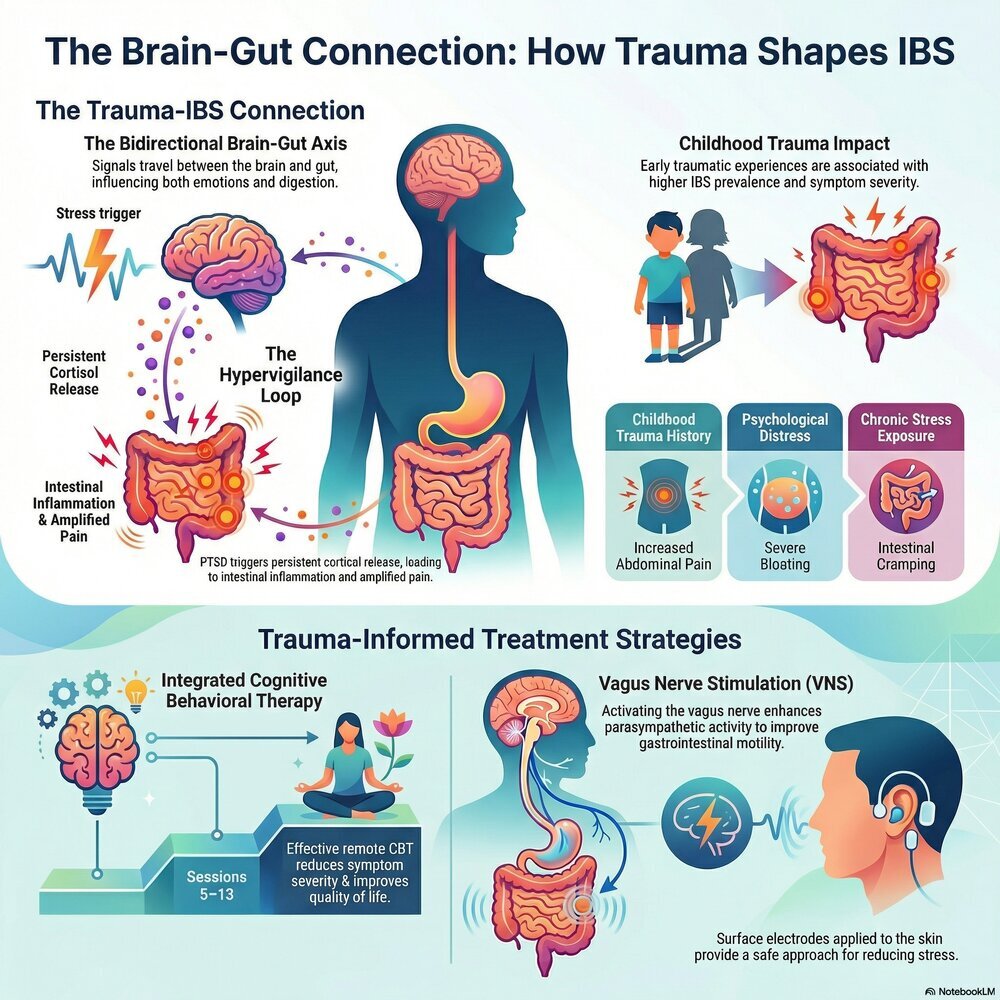
Common Manifestations: Bloating, Cramping, and Stress-Induced Flare-ups
A recent study of 436 IBS patients found that patients who experienced trauma as children were more likely to experience psychological distress that manifested as physical symptoms of pain, bloating, and cramping. This research highlights manifestations of stress-induced IBS and the need for trauma-informed treatment approaches for patients with histories of chronic psychological stress and trauma.
The Gut-Brain Axis: The Science of the Trauma-IBS Connection
Chronic stress alters intestinal sensitivity, motility, and permeability, contributing to conditions such as IBS. In turn, signals from the gut influence the brain, affecting behavior and emotions. This two-way interaction explains why stress and psychological states can worsen digestive conditions and lead to physical symptoms such as pain, bloating, diarrhea, and cramping.
PTSD and GI Symptoms: Why the Body "Keeps the Score"
A Holistic Path to Healing: Trauma-Informed Care for IBS
Beyond Diet: Integrating Stress Management into GI treatment
Vagus Nerve Stimulation: Techniques to Calm the Nervous System
- Chang L. (2011). The role of stress on physiologic responses and clinical symptoms in irritable bowel syndrome. Gastroenterology, 140(3), 761–765. https://doi.org/10.1053/j.gastro.2011.01.032
- Cohen, S., Murphy, M. L. M., & Prather, A. A. (2019). Ten Surprising Facts About Stressful Life Events and Disease Risk. Annual review of psychology, 70, 577–597. https://doi.org/10.1146/annurev-psych-010418-102857
- Dong, Z., Wang, X., Xuan, L., Wang, J., Zhan, T., Chen, Y., Xu, S., & Ji, D. (2025). The interaction effect between childhood trauma and negative events during adulthood on development and severity of irritable bowel syndrome. BMC gastroenterology, 25(1), 321. https://doi.org/10.1186/s12876-025-03919-7
- Kim, H., Oh, Y., & Chang, S. J. (2022). Internet-Delivered Cognitive Behavioral Therapy in Patients With Irritable Bowel Syndrome: Systematic Review and Meta-Analysis. Journal of medical Internet research, 24(6), e35260. https://doi.org/10.2196/35260
- Lakhan, S. E., & Kirchgessner, A. (2010). Neuroinflammation in inflammatory bowel disease. Journal of neuroinflammation, 7, 37. https://doi.org/10.1186/1742-2094-7-37
- Larauche, M., Mulak, A., & Taché, Y. (2012). Stress and visceral pain: from animal models to clinical therapies. Experimental neurology, 233(1), 49–67. https://doi.org/10.1016/j.expneurol.2011.04.020
- Margolis, K. G., Cryan, J. F., & Mayer, E. A. (2021). The Microbiota-Gut-Brain Axis: From Motility to Mood. Gastroenterology, 160(5), 1486–1501. https://doi.org/10.1053/j.gastro.2020.10.066
- Pacheco, R. L., Roizenblatt, A., Góis, A. F. T., Latorraca, C. O. C., Mota, C. F. M. G. P., & Riera, R. (2019). What do Cochrane systematic reviews say about the management of irritable bowel syndrome?. Sao Paulo medical journal = Revista paulista de medicina, 137(1), 82–91. https://doi.org/10.1590/1516-3180.2018.053740119
- Pitman, R. K., Rasmusson, A. M., Koenen, K. C., Shin, L. M., Orr, S. P., Gilbertson, M. W., Milad, M. R., & Liberzon, I. (2012). Biological studies of post-traumatic stress disorder. Nature reviews. Neuroscience, 13(11), 769–787. https://doi.org/10.1038/nrn3339
- Qin, H. Y., Cheng, C. W., Tang, X. D., & Bian, Z. X. (2014). Impact of psychological stress on irritable bowel syndrome. World journal of gastroenterology, 20(39), 14126–14131. https://doi.org/10.3748/wjg.v20.i39.14126
- Schubach, A., Quigley, B. M., Lackner, J. M., & Gudleski, G. D. (2024). Somatization Mediates the Relationship Between Childhood Trauma and Pain Ratings in Patients with Irritable Bowel Syndrome. Journal of clinical gastroenterology, 58(10), 1034–1042. https://doi.org/10.1097/MCG.0000000000001974
- Veldman, F., Hawinkels, K., & Keszthelyi, D. (2025). Efficacy of vagus nerve stimulation in gastrointestinal disorders: a systematic review. Gastroenterology report, 13, goaf009. https://doi.org/10.1093/gastro/goaf009





















Comments
Join The Conversation...