What Happens in the Vagus Nerve Doesn’t Stay There: Understanding Its Role in Gut Health
AKA: What happens in vagus…doesn’t stay in vagus.
The vagus nerve is one of the most fascinating—and important—communication highways in the body, especially when it comes to digestion.
Let’s start with a few quick facts.
The vagus nerve is the 10th and longest cranial nerve, historically referred to as the pneumogastric nerve because of its role in both breathing and digestion. The word vagus means “wandering” in Latin, which is fitting—it begins in the brain and travels all the way down into the abdomen, interacting with multiple organs along the way.
It plays a role in functions from the tongue to the intestines—and everything in between.
Fun fact: There are 12 pairs of cranial nerves in total, all originating from the brain, but the vagus nerve has one of the most widespread and impactful roles in the body.
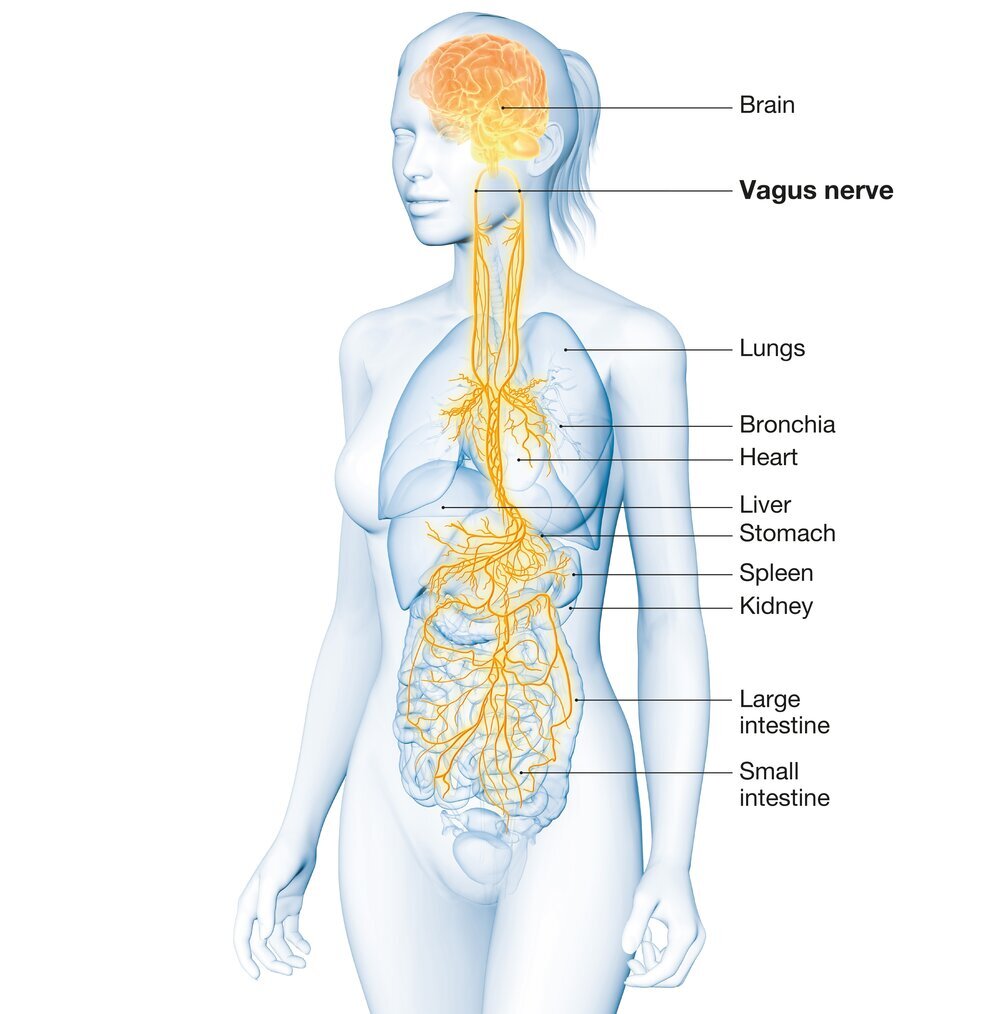
The Vagus Nerve: More Than Just Digestion
The vagus nerve has four primary functions:
- Sensory
- Motor
- Special sensory (including taste near the base of the tongue)
- Parasympathetic
From a gastrointestinal perspective, its responsibilities are extensive.
It provides sensory input from the larynx, esophagus, and much of the digestive tract, while also driving motor function—meaning the muscle contractions that move food through the GI tract.
It is also a key player in the parasympathetic nervous system, often referred to as the “rest and digest” system.
To simplify:
- The sympathetic nervous system = “fight or flight.”
- The parasympathetic nervous system = “rest and digest.”
The vagus nerve helps regulate that balance, which is critical for healthy digestion.
Why the Vagus Nerve Matters for Gut Health
The vagus nerve is deeply involved in how your body processes and moves food.
When it’s functioning well, it helps:
- Coordinate swallowing
- Support stomach acid production
- Regulate digestion
- Move food through the intestines
But when vagal function is impaired, symptoms can show up throughout the digestive tract.
Upper GI Effects
At the beginning of the digestive tract, impaired vagus nerve function may reduce esophageal muscle tone, making it harder to move food efficiently into the stomach.
In more severe cases, this can increase the risk of food entering the airway instead of the esophagus.
Stomach and Acid Regulation
The vagus nerve also plays a role in regulating stomach acid.
If it becomes dysregulated, the body may produce:
-
Too much acid, which can contribute to irritation, reflux, or GERD
-
Too little acid, which can impair digestion and lead to symptoms like bloating, nausea, diarrhea, and even nutrient deficiencies
Both ends of the spectrum can create digestive discomfort—just in different ways.
Intestinal Movement and IBS
Because the vagus nerve helps regulate intestinal motility, disruptions can also affect motility.
This may present as:
- Slower movement → constipation
- Irregular signaling → bloating or discomfort
And this is where the gut-brain axis becomes especially relevant.
The vagus nerve is a key connection point between the brain and the gut, meaning emotional and psychological stress can directly influence digestive symptoms.
For individuals with IBS, this connection is particularly important. Changes in stress levels, anxiety, or overall nervous system balance can amplify symptoms—even when diet remains consistent.
The Bigger Picture: The Gut-Brain Connection
The vagus nerve is one of the main pathways in the
gut-brain axis, the bidirectional communication system between your brain and digestive system.
This means:
- Your brain can influence your gut
- Your gut can influence your brain
It also explains why stress management, relaxation techniques, and overall nervous system support can play a meaningful role in managing conditions like IBS and even GERD.
Final Thoughts
The vagus nerve does far more than most people realize.
From swallowing to stomach acid production to intestinal movement—and even how stress affects your gut—it plays a central role in digestive health.
When something feels “off” in the gut, it’s not always just about food. Sometimes it’s about how the body communicates internally.
Understanding that connection is a powerful step toward more effective, whole-body digestive care.
-
Breit, S., Kupferberg, A., Rogler, G., & Hasler, G. (2018). Vagus nerve as modulator of the brain–gut axis in psychiatric and inflammatory disorders. Frontiers in Psychiatry, 9, 44. https://doi.org/10.3389/fpsyt.2018.00044
-
Bonaz, B., Bazin, T., & Pellissier, S. (2018). The vagus nerve at the interface of the microbiota–gut–brain axis. Frontiers in Neuroscience, 12, 49. https://doi.org/10.3389/fnins.2018.00049
-
Camilleri, M. (2012). Integrated upper gastrointestinal response to food intake. Gastroenterology, 131(2), 640–658.
-
Mayer, E. A. (2011). Gut feelings: The emerging biology of gut–brain communication. Nature Reviews Neuroscience, 12(8), 453–466. https://doi.org/10.1038/nrn3071























Comments
Join The Conversation...